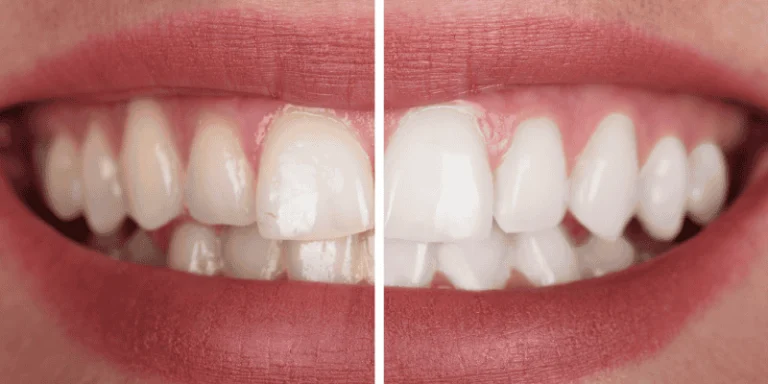
You can lighten your smile without trading comfort for brightness. Many whitening methods now include gentler formulas, desensitizing gels, or dentist‑supervised options that cut risk and reduce pain.
You can achieve teeth whitening for sensitive teeth safely by selecting low‑irritant products or professional treatments that protect both enamel and nerves.
If sensitivity concerns you, this guide explains why whitening can cause sensitivity and which choices reduce that risk.
You will learn simple at‑home steps, pro options that work with sensitivity, and quick tips to ease discomfort before, during, and after treatment.
Key Takeaways
- Choose gentle formulas or professionally guided treatments to protect sensitive teeth.
- Use desensitizing products and short, controlled whitening sessions.
- Talk to a dentist before whitening to reduce pain and avoid harm.
What Causes Sensitivity During Teeth Whitening?
You may feel sharp or tingling pain during or after teeth whitening because the treatment can reach tiny channels in your teeth, affect exposed root surfaces, or irritate gum tissue. Knowing the main causes helps you pick safer options and reduce pain quickly.
Enamel Erosion and Enamel Loss
Enamel is the hard outer layer that protects dentin. If your enamel is thin due to acid erosion, aggressive brushing, or wear, whitening agents can penetrate to the dentin more easily. That allows bleaching chemicals to reach nerve endings and causes short, sharp sensitivity.
Look for signs like translucent or yellowish tips and increased sensitivity to cold. You can help protect enamel by using fluoride treatments or desensitizing toothpaste before whitening.
Avoid whitening products with very high peroxide concentration if your enamel is already thin. Your dentist can measure enamel thickness and suggest a gentler method if needed.c
Gum Recession as a Sensitivity Trigger
When gums pull back, the root surfaces become exposed. Roots lack enamel and show dentin directly, so they react more to temperature and chemicals. Whitening gels touching these exposed areas often cause intense discomfort.
If you have receding gums from brushing too hard or gum disease, tell your dentist before whitening. Simple fixes like placing less gel near the gum line or using custom trays that fit correctly can reduce contact with roots. You might also need a professional cleaning or gum care first to lower the risk of long-lasting pain.
Effect of Whitening Agents on Sensitive Teeth
Whitening products mainly use hydrogen peroxide or carbamide peroxide to break stain molecules. These molecules can pass through enamel and dentin and temporarily inflame nerve endings inside the tooth. Stronger concentrations and longer exposure increase the chance of sensitivity.
Over-the-counter strips and DIY kits often sit on teeth without a perfect seal, which lets gel touch gums and exposed roots. Dentist-supervised treatments usually use lower concentrations or custom trays to control gel placement.
If you already have sensitive teeth, ask for sensitivity-specific formulas or shorter application times to cut down on pain.
Visit our Evansville, IN dental office to explore gentle whitening treatments designed specifically for patients with sensitive teeth.
How to Whiten Sensitive Teeth Safely
You can reduce pain and get visible whitening by choosing the right method, checking your mouth first, and using desensitizing products before treatment. Focus on professional guidance, fixing dental problems, and gradual whitening steps to keep sensitivity low.

Consulting with a Cosmetic Dentist
See a cosmetic dentist before any whitening. They will examine your teeth and gums, take X-rays if needed, and tell you which safe whitening options fit your case. If you have cavities, gum disease, or cracked teeth, the dentist will treat those first so whitening won’t make pain worse.
Ask about in-office treatments that use lower peroxide concentrations or violet LED activation, which some dentists use to reduce heat and sensitivity during bleaching. Get clear instructions about how long each session should last and whether you need take-home trays made from impressions of your teeth.
Bring a list of your current products and past whitening attempts. This helps the dentist choose a plan, professional single-visit whitening, custom trays for home use, or over-the-counter strips, based on what will likely reduce sensitivity while giving results.
Importance of Pre-Whitening Checks
Before whitening, check for decay, worn enamel, and exposed dentin. These issues make sensitivity worse and can produce poor whitening results. The dentist or hygienist will clean your teeth and point out any areas where enamel is thin or dentin shows through.
You may need fluoride varnish or a colored filling before whitening to seal exposed dentin. This step lowers the chance of sharp pain during treatment. Testing a small patch of tooth with a low-strength product first also helps predict how your teeth will react.
Make sure your dentist documents tooth shade and gum health. That record guides treatment intensity and timing. It also helps you track progress without overdoing peroxide exposure that can increase sensitivity.
Using Desensitizing Treatments Before Whitening
Desensitizing treatments can cut pain before and after whitening. Your dentist may apply a fluoride varnish, potassium nitrate gel, or a stannous fluoride product to block nerve signals and strengthen enamel. Use the exact product and schedule the dentist recommends.
You can also use desensitizing toothpaste containing potassium nitrate for 2–4 weeks before whitening. Brush twice daily; stop abrasive whitening pastes. If you have custom trays, your dentist can fit a desensitizing gel into them for short daily sessions before starting peroxide gel.
Follow all timing rules: don’t let peroxide sit longer than advised, and space treatments so your teeth recover. If sensitivity spikes, pause whitening and return to your desensitizing routine or contact your dentist for an adjusted plan.
Contact All In The Family Dental to find out which teeth whitening for sensitive teeth methods offer the best results while minimizing irritation and protecting your enamel.
Professional Teeth Whitening Options for Sensitive Teeth
Professional options aim to reduce sensitivity while giving predictable shade changes. You can get quick results with in-office care, or steady, gentler whitening at home using dentist-made trays and gels.
Professional In-Office Whitening
In-office whitening is performed in a dental office by a trained clinician. Your dentist will protect your gums and may apply a desensitizing agent before treatment to cut nerve irritation.
Treatments often use higher-strength peroxide and special lights or heating; this speeds whitening and lets the dentist stop if sensitivity rises.
Expect a single visit to lighten teeth by several shades. The dentist monitors your comfort and can pause between applications. If you already have strong sensitivity, ask about extra desensitizing steps or shorter application times.
Benefits:
- Fast, noticeable whitening in one visit
- Clinical monitoring to reduce risk of pain
- Desensitizing agents available before/during/after
Custom Take-Home Trays and Kits
Custom trays come from molds your dentist takes of your teeth. These trays fit snugly and spread professional-grade gel evenly, which reduces gum contact and lowers sensitivity compared with one-size-fits strips.
You wear trays for a set time each day or overnight, based on your dentist’s plan. This gradual approach lets you control how fast your teeth whiten. Your dentist can supply a gel with lower peroxide or add a desensitizing formula to the regimen.
Practical points:
- Better fit = less gum irritation
- Adjustable wear time to manage sensitivity
- Refillable gels for longer maintenance
Professional-Grade Whitening Gel
Professional gels use higher-quality active ingredients than most over-the-counter products. Dentists choose concentrations and formulations (hydrogen peroxide or carbamide peroxide) to match your sensitivity level.
Many gels are paired with desensitizing agents like potassium nitrate or fluoride to calm nerves and strengthen enamel. Your dentist can recommend low-peroxide options or PAP-based alternatives if peroxide aggravates your teeth.
What to ask your dentist:
- Gel concentration and ingredients
- Whether a desensitizing additive is included
- Recommended wear schedule and follow-up care
Gentle At-Home Whitening Solutions
You can reduce stains without triggering sharp sensitivity by choosing lower-strength products and using them as directed. Look for enamel-friendly ingredients and short daily contact times to limit discomfort.
Whitening Toothpaste for Sensitive Teeth
Whitening toothpaste for sensitive teeth uses mild abrasives or nano-hydroxyapatite instead of high peroxide levels. These formulas polish surface stains and help rebuild enamel, which lowers sensitivity over time.
Pick a toothpaste that lists “sensitive” on the label and includes ingredients like potassium nitrate or nano-hydroxyapatite.
Use the toothpaste twice daily for maintenance. Expect gradual results over weeks, not days. It works best after you finish stronger treatments to keep stains from returning. If your toothpaste causes tingling, stop and try a different brand.
Benefits:
- Daily use fits into your routine.
- Low risk of causing new sensitivity.
- Helps protect enamel while reducing surface stains.
Limitations:
- Not as fast or dramatic as strips or kits.
- Results are subtle and need consistent use.
Try pairing whitening toothpaste with a soft-bristled brush and short, gentle strokes to protect enamel and gums.
Whitening Strips for Sensitive Teeth
Whitening strips for sensitive teeth use lower peroxide concentrations or alternative, gentler formulas to reduce sensitivity. They deliver noticeable whitening over 1–2 weeks while aiming to limit nerve irritation. Choose strips labeled for sensitivity and follow the recommended wear time exactly.
Apply strips to clean, dry teeth and press to remove air bubbles. Avoid touching the gums; excess gel can cause irritation. If you feel sharp pain, remove the strip and rinse. Some gentle strips use peroxide-free formulas or include soothing agents such as coconut extract or glycerin.
Pros:
- Clear step-by-step use.
- Portable and usually affordable.
- Many options made for sensitivity control.
Cons:
- May slip on bottom teeth.
- Results vary; deep stains need stronger options.
For product details and comparisons, review trusted reviews of whitening strips designed for sensitive teeth to find the formula that fits your needs, like options tested by experts.
Over-the-Counter Whitening Kits
Over-the-counter whitening kits include trays, syringes of gel, or LED-enhanced strips made for home use. For sensitive teeth look for lower peroxide levels (commonly 6–10% carbamide peroxide or lower) and clear instructions about wear time.
Some kits add desensitizing agents to the gel to help prevent post-treatment pain.
You can use tray-based kits with custom-fit trays when available, but poor-fitting trays can push gel onto gums and raise irritation risk. LED lights may speed results but don’t eliminate sensitivity risks. Always follow the shortest effective schedule and stop if you get persistent pain.
Checklist before buying:
- Label indicates “sensitive” or low peroxide.
- Clear wear-time instructions.
- Includes desensitizing ingredient or post-care guidance.
If you have dental work, cracked teeth, or severe sensitivity, consult your dentist before using any over-the-counter whitening kit.
Contact All In The Family Dental to learn how safe whitening solutions can brighten your smile while keeping sensitivity under control.
Natural and Alternative Teeth Whitening Remedies
You can try gentle home methods that may reduce surface stains and help with mild discoloration. These options work best when you have healthy enamel and no active tooth problems.
Oil Pulling with Coconut Oil
Oil pulling uses a tablespoon of coconut oil swished around your mouth for 10–20 minutes. Do this in the morning before eating or brushing. It may reduce surface stains and lower bacteria that cause bad breath and plaque.
Use cold‑pressed, unrefined coconut oil. Spit into a trash can (not the sink) to avoid clogging pipes. Stop if you feel jaw pain or nausea. Oil pulling is not a bleach, expect small, gradual changes over weeks, not instant whitening.
If you have gum disease, cavities, or very sensitive teeth, talk to your dentist before starting. Combine oil pulling with regular brushing using a toothpaste for sensitivity for best results.
Hydrogen Peroxide Rinse
A diluted hydrogen peroxide rinse can help lift surface stains. Mix equal parts 3% hydrogen peroxide and water for a 1.5% rinse, swish for 30–60 seconds, then spit. Do this no more than twice a week to avoid irritating gums or enamel.
Do not swallow the rinse. Rinse with plain water after and wait at least 30 minutes before brushing to avoid increased abrasion. If your gums sting or your teeth feel more sensitive, stop and consult your dentist.
This method treats surface discoloration only. For deeper stains or faster results, dentist‑supervised whitening is safer and more effective.
Lifestyle and Dietary Habits for a Whiter Smile
Change what you eat and how you drink to reduce new stains. Cut back on coffee, tea, red wine, and dark sodas. Use a straw for beverages when possible to limit contact with front teeth.
Brush twice daily with a soft brush and toothpaste for sensitivity. Floss daily to remove stain‑holding plaque between teeth. Eat crunchy fruits and veggies like apples and carrots to help scrub teeth naturally.
Avoid acidic foods and hard scrubbing, which wear enamel and increase sensitivity. See your dentist for professional cleaning every six months to remove stubborn surface stains and check that home methods are safe for your teeth.
Tips for Minimizing Sensitivity During and After Whitening
Use targeted products, gentle brushing, and simple aftercare steps to cut pain and protect enamel. Small daily choices, like the right toothpaste and brush, make whitening more comfortable and keep results longer.
Using Desensitizing Toothpaste
Choose a toothpaste with potassium nitrate or stannous fluoride to block nerve signals and reduce short-term pain. Use it twice a day starting a week before whitening and continue for at least two weeks after treatment.
Apply a pea-sized amount and brush gently for two minutes. You can also apply a dab directly to sensitive spots and leave it on for a minute before rinsing to get faster relief.
Look for specific product claims if you want whitening plus sensitivity care. For example, Sensodyne Extra Whitening combines sensitivity protection with mild stain removal; it won’t whiten as much as peroxide kits but it helps prevent post-whitening zing.
If you still feel strong sensitivity, stop whitening and talk to your dentist about professional desensitizing agents or a prescription-strength toothpaste.
Choosing a Soft-Bristled Toothbrush
Pick a soft-bristled toothbrush to avoid scrubbing away enamel and irritating gums. Soft nylon bristles clean well when used with light pressure; avoid medium or hard brushes that increase sensitivity.
Use a toothbrush with a small head so you can reach back teeth and clean along the gumline without forcing the brush. Consider an electric toothbrush with pressure sensors, these help keep your strokes gentle and consistent.
Replace the brush every 3 months or sooner if bristles fray. Frayed bristles clean poorly and make you press harder, which raises the risk of gum recession and exposed dentin.
When brushing after whitening, wait 30 minutes to let your saliva neutralize acids. Then brush gently with your soft brush and desensitizing toothpaste.
Aftercare to Maintain Results and Comfort

Rinse with plain water right after whitening to remove leftover gel. Avoid hot, cold, acidic, or staining foods for 24–48 hours, this lowers sensitivity and preserves whitening effects.
Use fluoride mouthwash or a remineralizing rinse nightly to rebuild enamel and reduce discomfort. If available, apply a fluoride gel or varnish at home or ask your dentist for an in-office application for stronger protection.
If you use at-home trays, follow the recommended wear time exactly. Overuse and higher peroxide concentrations raise the chance of nerve irritation and gum damage.
Track sensitivity on a scale of 0–10. If it stays above 5 after 48 hours, pause whitening and contact your dentist. They can offer tailored care like in-office desensitizing treatments or change your whitening plan.
Not sure which whitening option is right for you? Schedule a visit to receive personalized recommendations based on your sensitivity level.
Frequently Asked Questions
This section explains safe whitening choices, ways to lower pain, which ingredients can cause trouble, how often to whiten, and whether home kits or natural options work for sensitive teeth.
What are the best teeth whitening options for people with sensitive teeth?
Professional in-office whitening lets your dentist control strength and protect your gums. Custom take-home trays from a dentist use lower-strength gel and fit tightly, which cuts gum contact and reduces sensitivity.
Desensitizing toothpastes and gels that contain potassium nitrate or fluoride help before and during whitening. Ask your dentist about products like Opalescence PF, which are designed to be gentler on sensitive teeth (example of a professional option).
How can I protect my sensitive teeth while whitening them?
Use a toothpaste for sensitive teeth for at least two weeks before you start whitening. This builds up protection and can reduce pain during treatment.
Have your dentist check for cavities, cracked teeth, or gum recession before whitening. Fixing these issues first prevents worse sensitivity and makes whitening safer.
Are there any natural remedies for whitening sensitive teeth?
Baking soda mixed with water can remove surface stains gently when used sparingly. Limit use to avoid wearing enamel.
Oil pulling and activated charcoal lack strong evidence and can be abrasive or messy. Talk with your dentist before trying natural methods to avoid harm.
How often should I whiten my teeth if they are sensitive?
Space professional or at-home treatments by several months if you notice increased sensitivity. Your dentist can suggest an interval based on the product strength and your response.
For touch-ups, use the weakest effective method and follow the product directions closely. Over-whitening raises the risk of lasting sensitivity.
What ingredients should I avoid in teeth whitening products for sensitive teeth?
Avoid high concentrations of hydrogen peroxide and carbamide peroxide unless a dentist supervises use. Strong peroxides increase sensitivity and can irritate gums.
Also avoid abrasive agents that scrub enamel, such as coarse charcoal or overly gritty pastes. These can wear enamel and expose dentin, which makes sensitivity worse.
Can I use over-the-counter teeth whitening kits if I have tooth sensitivity?
You can, but choose low-strength gels and avoid daily use unless the product is made for sensitive teeth. Look for kits labeled for sensitivity or containing desensitizing agents.
Better options include dentist-provided custom trays or a supervised in-office treatment. If you try an OTC kit and pain starts, stop and see your dentist.