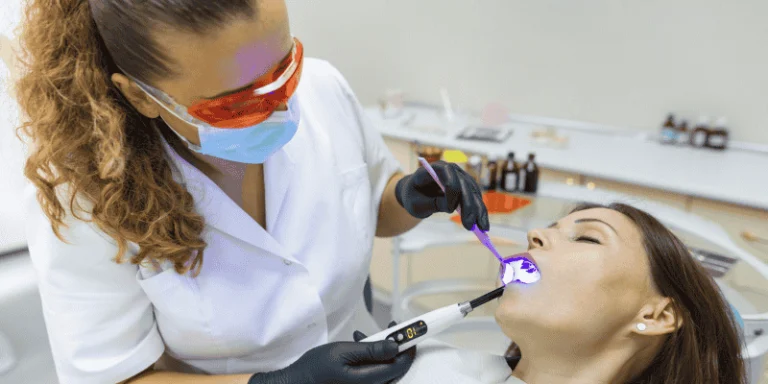
Long dental procedures can feel overwhelming, but you don’t have to face them stressed or in pain.
Sedation dentistry for long procedures helps you stay calm and comfortable during long treatments, while your dental team monitors you closely and controls your level of awareness.
You’ll learn which sedation options fit your health and procedure, how the meds work, and what to expect before, during, and after your appointment. This guide helps you prepare so the visit feels simpler and safer.
Key Takeaways
- Sedation helps you stay calm and comfortable during long dental procedures.
- Different sedation modalities correspond to different needs and procedure durations.
- Your team will monitor your safety and give recovery instructions.
Sedation Dentistry for Long Procedures: The Essentials
Long dental visits can be stressful, but there are options to help you stay calm, comfortable, and safe. This section explains who typically benefits and exactly how different sedation levels work, so you can talk with your dentist with confidence.
Who Can Benefit from Sedation Dentistry
You may benefit from sedation dentistry if you have strong dental anxiety, a sensitive gag reflex, or need multiple treatments in one visit, like implants, bone grafts, or full-mouth restorations. Patients with limited ability to sit still, due to a disability, severe TMJ pain, or long medical conditions, also find sedation helpful.
Discuss your medical history and current medications with your dentist. Certain conditions (like uncontrolled sleep apnea or recent heart problems) change which sedation is safe.
Your dentist will assess risks and suggest options such as nitrous oxide, an oral sedative, IV sedation, or general anesthesia for very complex surgery.
Bring a companion if you expect oral, IV, or deep sedation. You’ll likely need someone to drive you home and stay with you until the grogginess passes. Follow pre-op instructions on fasting and medicines carefully to reduce complications.
Levels of Sedation Explained
Sedation ranges from minimal (you stay fully awake but relaxed) to general anesthesia (you are fully unconscious). The common levels are:
- Minimal sedation (nitrous oxide or low-dose oral): You feel relaxed and remain responsive. Recovery is fast; you can often drive after nitrous oxide.
- Moderate (conscious) sedation (oral or IV): You’re very drowsy and may not remember much. You can still respond to commands. Plan for a ride home and several hours of recovery.
- Deep sedation: You are on the edge of consciousness and may not respond. Monitoring of breathing and vital signs is essential.
- General anesthesia: You are completely asleep and require an anesthesiologist and post-op monitoring. Used for major surgeries or when other methods aren’t safe.
Your dentist will match the sedation level to the procedure length, your anxiety, and your health. They’ll monitor heart rate, oxygen levels, and blood pressure throughout to keep you safe.
Types of Sedation and How They Work
You will learn the main sedation choices used for long dental procedures, how each one is given, what you feel, and key safety steps to plan for. Pay attention to preparation, recovery time, and whether you need someone to drive you home.
Oral Sedation
Oral sedation uses pills you take before the appointment to reduce anxiety and make you drowsy. Common drugs include benzodiazepines such as triazolam or diazepam. Your dentist will tell you the exact dose and when to take it, usually about one hour before the procedure.
You will stay awake but relaxed and may have limited memory of the visit. Effects can last several hours, so arrange a responsible adult to drive you home and stay with you for a few hours. Avoid alcohol, certain medications, and heavy meals before taking oral sedatives.
Your medical history and current medicines matter. Tell your dentist about sleep apnea, liver disease, or drugs that interact with benzodiazepines. The team will monitor your breathing and oxygen levels during the procedure.
Visit our Evansville, IN dental office to explore safe sedation dentistry options designed for longer or more complex dental procedures.
Nitrous Oxide (Laughing Gas)
Nitrous oxide, often called laughing gas, is an inhaled minimal sedation delivered through a nasal mask. It works quickly; you usually feel calmer within minutes. Your dentist adjusts the gas mix so you stay awake but relaxed.
Effects wear off almost immediately when the mask is removed. Most patients can drive themselves home and resume normal activity right away. Nitrous oxide suits people with mild to moderate anxiety and those who need short or moderately long procedures.
Side effects are rare but can include lightheadedness or nausea. You should tell your dentist if you have a recent cold, respiratory problems, or vitamin B12 deficiency, as those can affect nitrous oxide use. The team will monitor your breathing and oxygen during use.
IV Sedation
IV sedation puts sedative drugs directly into your bloodstream for faster, deeper relaxation. This often uses medications from the benzodiazepine family or other sedative agents. Your level of awareness ranges from very drowsy to nearly unresponsive, depending on dose.
IV sedation is adjustable during the procedure, which makes it useful for long, complex work like implants or multiple extractions. Expect little memory of the treatment afterward. You will need someone to drive you home, and you’ll remain under observation until staff judge you safe to leave.
Because the sedatives act quickly and strongly, the team will monitor heart rate, blood pressure, oxygen saturation, and, when indicated, capnography-derived measures of breathing. Share all health details and current medications beforehand so the dentist or anesthetist can plan the safest dose.
General Anesthesia for Dentistry
General anesthesia makes you fully unconscious and is reserved for major oral surgery or patients who can’t tolerate lighter methods. An anesthesiologist or trained provider usually gives it, often in a hospital or surgical center setting.
You will not feel or remember the procedure. Recovery takes longer than other sedations, and you will need close monitoring for breathing, circulation, and wake-up. Arrange for post-op care and follow fasting rule, typically 6–8 hours without food or drink before anesthesia.
General anesthesia carries higher risks than other sedation methods, so providers review your medical history, allergies, and medications in detail. They will explain the specific risks and give written pre-op and post-op instructions you must follow.
Benefits and Considerations of Sedation Dentistry
Sedation can reduce fear, lower pain, and help you sit still for long work. It affects breathing, memory, and recovery time in different ways depending on the method used.

Managing Dental Anxiety and Phobia
If you feel panic, nausea, or frozen muscles at the thought of the dentist, sedation can help you stay calm.
Nitrous oxide (laughing gas) eases anxiety quickly and wears off fast, so you can go home the same day without a ride in many cases.
Oral sedatives like triazolam or diazepam give deeper relaxation; you may feel drowsy and should arrange for someone to drive you.
Your dentist will review your medical history, current meds, and weight to pick a safe option. Be honest about past reactions to medicines, sleep apnea, or heart problems. These details change which sedation is safe and how your vitals are monitored during treatment.
Making Long Procedures Comfortable
For multi-hour work, implants, extractions, or full-mouth rehab, IV sedation or deeper oral sedation helps you tolerate longer visits.
IV sedation gives precise control over how relaxed you are, so the team can adjust dose during the procedure for steady comfort. That often reduces the number of visits and the physical stress of repeated appointments.
Expect longer recovery after moderate or deep sedation. You may be groggy for several hours and need a companion to take you home. Your team will monitor oxygen and heart rate and give clear pre- and post-op instructions, like fasting rules and medication pauses, to keep you safe.
Impact on Sensitive Teeth and Gag Reflex
Sedation eases sensitivity by lowering your anxiety and pain perception, which helps if local anesthetic alone doesn’t fully numb tender teeth. When you relax, your muscles loosen and you may jaw more easily, making injections and dental work simpler.
If you have a strong gag reflex, sedation can relax throat muscles and reduce gagging during impressions, crowns, or lengthy cleanings. Nitrous oxide helps mild to moderate gag reflexes. For severe gagging, deeper sedation or IV options often work better because they suppress the reflex more reliably.
Not sure if sedation dentistry is right for you? Call our experts to discuss your procedure, comfort needs, and sedation options.
Safety Measures in Sedation Dentistry
You will learn how clinics check your health, watch your breathing and circulation, and which trained professionals run the sedation. These steps reduce risk and keep you comfortable during long procedures.
Patient Screening and Medical History

Clinics start with a full medical review before any sedation procedure. You will be asked about past surgeries, heart or lung problems, sleep apnea, allergies, and current medications, including over‑the‑counter and herbal supplements. Tell your team about smoking, alcohol use, and recent illness.
The American Dental Association recommends using standardized screening to match sedation level to your health. For example, deep sedation or general anesthesia may require clearance from a physician if you have heart disease or uncontrolled diabetes.
You may need blood pressure checks, an EKG, or lab tests before the appointment. Fasting rules also matter: most offices ask you not to eat solids for 6–8 hours and to limit clear liquids up to 2 hours before some sedations. Follow these instructions exactly to lower the chance of aspiration or other complications.
Vital Signs Monitoring
During the procedure, staff continuously track your breathing, oxygen levels, heart rate, and blood pressure. You will typically wear a pulse oximeter to monitor oxygen saturation and an automatically cycling blood pressure cuff.
Capnography, a monitor that measures exhaled carbon dioxide, is standard for moderate to deep sedation and can detect breathing problems more quickly than oxygen saturation alone.
Trained team members assess your level of consciousness and breathing pattern by observing and speaking to you as appropriate. Reversal drugs and oxygen are kept immediately available. Clinics use checklists to document readings at regular intervals, so any changes are caught quickly and addressed.
Role of Dental Teams and Anesthesiologists
Your care team often includes a dentist trained in sedation, a certified sedation nurse or dental assistant, and, for deeper sedation, an anesthesiologist or a dentist with anesthesia credentials.
Each person has a clear role: the operator performs the dental work while another clinician focuses solely on monitoring and airway management.
Professional groups like the American Dental Society of Anesthesiology set training and equipment standards many practices follow. Team members maintain certifications in advanced cardiac life support (ACLS) or pediatric advanced life support when treating children.
They also run emergency drills and keep resuscitation drugs and a defibrillator on site so they can respond immediately if needed.
Preparing for Your Sedation Dentistry Appointment
You will need to follow clear fasting and medication rules, arrange a driver, and bring ID plus a list of meds. Dress comfortably and plan for rest and soft foods at home.
Pre-Procedure Instructions
Follow your dentist’s exact fasting rules. For oral or IV sedation, don’t eat or drink for 6–8 hours before the appointment. For nitrous oxide, avoid heavy meals for a few hours.
Tell your dentist every prescription, over-the-counter drug, and supplement you take. Blood thinners, certain diabetes meds, and herbal supplements can change sedation plans. Ask whether to take your usual morning medications with a small sip of water.
Share medical history details like heart, lung, liver, or kidney problems and any previous reactions to sedatives. If you have sleep apnea, bring that up, your dentist may change the sedation level. Follow any specific breathing or mouth-rinse instructions the office gives the day of the procedure.
What to Bring and Arrange Beforehand
Arrange a responsible adult to drive you home and stay with you for several hours. You’ll be drowsy and your judgment and reflexes will be impaired.
Bring a printed list of your current medications and allergies, your ID, and your insurance card. Leave jewelry and contact lenses at home. Wear loose clothing and a short-sleeve shirt if you may receive an IV.
Plan your post-care: stock soft foods (yogurt, soup, applesauce), have pain meds approved by your dentist on hand, and clear your schedule for the rest of the day. Keep your phone charged and save your dentist’s phone number for any questions after you leave.
What to Expect During and After Sedation
You will feel relaxed and monitored the whole time. Staff will watch your breathing, heart rate, and oxygen, and they will tell you what to expect at each step.
What Happens During the Procedure
You’ll arrive with a companion who can drive you home. The team will review your medical history and confirm any medications. If you get IV sedation, a small IV goes in your arm; for oral sedation, you’ll take a pill before the procedure; for nitrous oxide, you’ll wear a nasal mask.
A monitor will track your heart rate, blood pressure, and oxygen. The dentist adjusts medication so you stay calm but safe. For long procedures like multiple dental implants, IV sedation often keeps you comfortable for hours without repeated dosing.
You may be drowsy or drift in and out of awareness. You usually won’t feel the drilling or pulling. Staff will check your comfort, give local anesthetic when needed, and pause if any issue arises.
Immediate Post-Procedure Recovery
Right after the procedure, staff move you to a recovery chair. They continue to watch your vitals until you reach a safe level of alertness. If you had nitrous oxide, the effects wear off in minutes and you may sit up and leave soon after.
With oral or IV sedation, expect drowsiness for several hours. You’ll need someone to escort you home and stay with you until you’re steady. Avoid driving, signing legal papers, or making major decisions for 24 hours.
The team will give written aftercare steps and note any follow-up visits, especially if you had extractions or implants placed during the appointment.
Post-Procedure Care and Aftereffects
Follow these common instructions: rest for the rest of the day, eat soft foods, and avoid alcohol or heavy machinery. For dental implant sites, keep the area clean with gentle rinses, salt water or dentist-recommended rinses, starting the day after surgery.
You may have mild nausea, lightheadedness, dry mouth, or memory gaps about the procedure. These are normal and often fade in hours to a day. Watch for warning signs like heavy bleeding, fever, severe swelling, or breathing trouble and contact your dentist or emergency services right away.
If you were given prescription pain meds or antibiotics, take them exactly as directed. Keep all follow-up visits so the dentist can check healing and remove sutures or adjust temporary restorations.
Contact All In The Family Dental to learn how sedation dentistry can help you complete long dental procedures comfortably and with peace of mind.
Frequently Asked Questions
You will find clear, practical answers about IV sedation, common drugs used, costs, insurance, risks, and recovery after a long dental procedure. Each answer tells you what to expect and how to prepare.
What can I anticipate during a dental procedure with IV sedation?
IV sedation starts with a small needle into a vein, usually in your hand or arm. The sedative works quickly, so you’ll feel relaxed within minutes.
You may stay semi-awake or drift in and out of sleep. Your breathing, heart rate, and blood pressure are monitored the whole time.
You usually won’t feel pain, and many people remember little or nothing after the procedure. Your dental team can adjust the medication level while you’re treated.
Which medications are commonly administered for IV sedation during dental treatments?
Common drugs include benzodiazepines such as midazolam and sometimes short-acting opioids for pain control. These medications reduce anxiety and cause drowsiness.
An anesthesiologist or trained dental provider chooses doses based on your weight, health, and the planned procedure length. They may also give local anesthetic so you don’t feel pain in the treated area.
How do costs for sedation dentistry typically break down?
Costs usually include the sedative drugs, monitoring equipment, and the provider’s anesthesia fee. You may also pay separate fees for the dental procedure itself and any facility or recovery room charges.
Longer procedures raise the anesthesia cost because more medication and monitoring time are needed. Ask for an itemized estimate before you book so you know each charge.
Will my dental insurance help cover the costs of sedation dentistry?
Some insurance plans cover sedation when it’s medically necessary, such as for major surgery or severe anxiety that prevents treatment. Other plans only cover nitrous oxide or may not cover sedation at all.
Contact your insurer with the procedure code and a written statement from your dentist explaining medical necessity. That increases the chance of partial reimbursement.
What are the potential risks associated with dental sedation?
Common short-term effects include drowsiness, nausea, and dry mouth. Your breathing and blood pressure can drop, so trained staff monitor you continuously.
Rare but serious risks include allergic reactions or problems with breathing that require emergency care. Your dental team will review your medical history and may require pre-op clearance if you have lung, heart, or sleep apnea issues.
How should I expect to feel after waking up from dental sedation following a long procedure?
You may feel groggy, confused, or sleepy for several hours after waking. Plan to rest the rest of the day and avoid driving, alcohol, or heavy decisions for 24 hours.
Some people feel mild nausea or lightheadedness; mild pain at the treated site is common once local anesthesia wears off. Follow your provider’s post-op instructions for fluids, food, and when to restart medications.