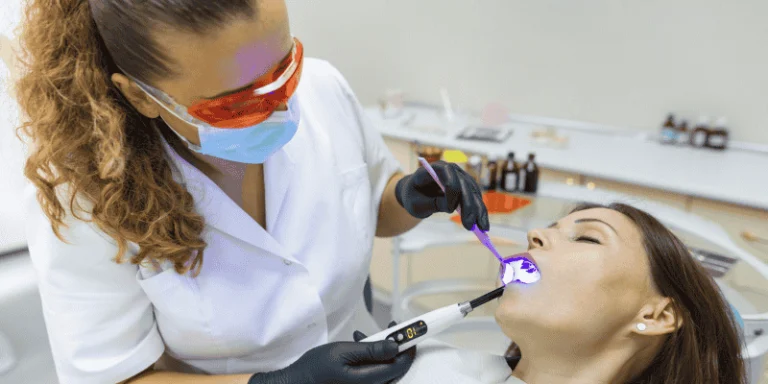
If you live with a heart condition, diabetes, asthma, or another medical issue, you may worry about how dental treatment will affect your health. You might even delay care because of fear or past bad experiences.
Sedation dentistry for medical conditions can offer safe, controlled treatment when your dental team carefully reviews your medical history and tailors the sedation to your specific health needs.
With the right plan, you can stay calm and comfortable while your vital signs are closely monitored throughout the visit.
When you understand your options and the safety steps involved, you gain more control over your care. Knowing what to expect helps you feel prepared and confident before you even sit in the dental chair.
Key Takeaways
- Sedation dentistry can be adjusted to match your specific medical condition.
- Careful health screening and monitoring help support your safety.
- The right approach can make dental visits calmer and more manageable.
Understanding Sedation Dentistry and Its Importance for Patients With Medical Conditions
Sedation can make dental care possible when fear, pain, or health problems make treatment hard. If you live with a medical condition, you need a plan that keeps you comfortable and safe during every visit.
What Is Sedation Dentistry?
Sedation dentistry uses medication to help you relax during dental treatment. You stay awake in most cases, but you feel calm and less aware of the procedure.
Common sedation options include:
- Nitrous oxide (laughing gas): You breathe it through a mask. It works fast and wears off quickly.
- Oral sedation: You take a pill before your visit. It helps reduce anxiety.
- IV sedation: The dentist gives medication through a vein for deeper relaxation.
Even with dental sedation, your dentist still uses local anesthesia to control pain. Safe sedation means trained staff, proper monitoring, and equipment to check your oxygen level, heart rate, and blood pressure during treatment.
Why Medical Conditions Require Special Sedation Considerations
If you have a medical condition, sedation is not one-size-fits-all. Your dentist must adjust the plan to protect your health.
Some conditions, such as high blood pressure, epilepsy, or Parkinson’s disease, can worsen with stress. Research on conscious sedation in dentistry shows that sedation can help control anxiety and reduce stress-related complications during treatment.
However, certain health issues raise risk. These include:
- Obesity or sleep apnea
- Chronic lung disease
- Multiple serious medical problems
- Pregnancy or drug allergies
You may need medical clearance before treatment. Your dentist will review your medications, past surgeries, and overall health. This careful screening supports safe sedation and lowers the risk of breathing problems or drug interactions.
For some patients, especially those with physical or developmental conditions, sedation dentistry for special needs allows care that would otherwise be unsafe or impossible.
How Medical Conditions Can Affect Oral Health
Medical conditions often change your oral health in direct ways. Some diseases increase your risk of infection, gum disease, or dry mouth.
For example:
- Diabetes can slow healing and raise gum disease risk.
- Heart disease may require antibiotic precautions.
- Autoimmune disorders can inflame oral tissues.
- Medications for blood pressure or depression may reduce saliva.
Dry mouth raises your risk of cavities because saliva protects your teeth. If you avoid the dentist due to anxiety or physical limits, problems can grow worse over time.
Sedation dentistry helps you receive regular cleaning and exams, fillings, and other care without severe stress. When your dentist understands your health history and selects the right sedation options, you can protect both your oral health and your overall health with greater confidence.
Medical Conditions Impacting Sedation Dentistry
Your medical history shapes how your dentist plans dental sedation. Heart, lung, blood sugar, and brain conditions can change which drugs are safe and how closely your team monitors you.
Cardiovascular Diseases and Sedation Considerations
If you have heart disease, stress control becomes a top priority. Anxiety can raise your heart rate and blood pressure, which may trigger chest pain in people with angina. In these cases, conscious sedation or minimal sedation can lower stress and reduce strain on your heart.
Stable angina and controlled high blood pressure often allow moderate sedation with careful monitoring. Your dentist will check your blood pressure before treatment. Very high readings may delay care or require a specialist setting.
If you had a recent heart attack, you may need to wait before receiving deep sedation. Oxygen support and close monitoring are often required for higher‑risk patients.
Respiratory Disorders and Airway Management
If you have asthma or chronic lung disease, your airway needs special attention. Some sedation drugs can slow breathing, especially during deep sedation. Your dentist must balance comfort with safe oxygen levels.
Well‑controlled asthma usually does not block you from receiving conscious sedation. You may need to bring your rescue inhaler and use it before treatment. Poorly controlled asthma may require treatment in a setting with advanced airway support.
Conditions like COPD increase the risk of low oxygen levels. Your team may provide supplemental oxygen and monitor your breathing closely.
According to research on conscious sedation in dentistry, patients must keep protective reflexes and breathe on their own during conscious sedation. If that cannot be assured, your dentist may adjust the plan.
Diabetes Management During Dental Sedation
If you have diabetes, stable blood sugar is essential before dental sedation. Long appointments and fasting can cause low blood sugar, which may lead to dizziness or confusion.
Your dentist may schedule your visit early in the day. You may need to eat a light meal and take your usual medication unless told otherwise. Always share your most recent blood sugar readings.
Moderate sedation can mask signs of low blood sugar. That makes pre‑treatment planning critical. Bring your glucose monitor and fast‑acting sugar to the appointment.
Poorly controlled diabetes may delay elective procedures. In some cases, your dentist may coordinate care with your physician before using deep sedation.
Neurological and Cognitive Disorders
If you live with epilepsy, movement disorders, or cognitive conditions, sedation can make dental care safer and easier. Stress can trigger seizures in some people, so conscious sedation may lower that risk.
However, seizure frequency matters. Poorly controlled epilepsy may require care in a specialized center. Some anti‑seizure drugs interact with sedatives, which can lead to weaker or stronger effects than expected.
Movement disorders can make it hard to stay still. Moderate sedation often reduces muscle activity and improves safety.
If you have memory loss or developmental conditions, your dentist will adjust the level of sedation. The goal stays the same: keep you comfortable while protecting your breathing and reflexes.
Sedation Options and Customization for Different Medical Needs
Your medical history shapes the type and level of sedation you can safely receive. Dentists adjust sedation methods, monitoring, and team support to match your health condition, medications, and treatment needs.
Overview of Sedation Methods: Nitrous Oxide, Oral, and IV Sedation
Dentists use three main types of sedation in dental sedation services: nitrous oxide, oral sedation, and IV sedation.
Nitrous oxide (laughing gas) works quickly and wears off fast. You breathe it through a small mask. It helps with mild anxiety and allows you to stay awake and responsive.
Many patients with controlled medical conditions tolerate it well because dentists can adjust the level during the visit.
Oral sedation involves taking a prescribed pill before your appointment. It creates a deeper sense of calm than nitrous oxide. You remain awake, but you may feel drowsy. Your dentist reviews your medications and liver function before choosing this option.
IV sedation goes through a vein and works quickly. It allows better control of sedation depth. Dentists often use it for patients with complex medical needs who require longer or more involved treatment.
Choosing the Right Sedation Level: Minimal, Moderate, and Deep
Sedation falls into three main levels: minimal, moderate, and deep sedation.
With minimal sedation, you feel relaxed but fully awake. Dentists often use nitrous oxide for this level. It works well if you have mild anxiety and stable health conditions.
Moderate sedation makes you more drowsy. You may not remember much of the procedure. Oral medications or IV sedation can create this level. Dentists choose it when anxiety, movement disorders, or medical issues make treatment harder to complete safely.
Deep sedation brings you close to sleep. You can still respond to strong stimulation, but you may not stay fully aware. This level requires advanced monitoring. Dentists consider your heart, lung function, and current diagnoses before recommending it.
Role of the Anesthesiologist and the Care Team in Assessment
An anesthesiologist or trained sedation provider plays a key role when you have complex medical conditions.
Before treatment, the team reviews your full medical history. They check your diagnoses, past surgeries, allergies, and current medications.
For high‑risk cases, practices that follow guidance on setting up dental sedation services for special care patients often use structured protocols and clear team roles.
During the procedure, the care team monitors your blood pressure, heart rate, oxygen level, and breathing. They adjust medication as needed. If you have heart disease, diabetes, respiratory illness, or a neurological condition, this close monitoring helps reduce risk.
You benefit most when your dentist, anesthesiologist, and primary physician share clear information and work together.
Pre-Procedure Evaluation and Safety Protocols
Before you receive dental anesthesia or other dental sedation services, your dental team must review your health in detail and prepare for possible risks. Careful screening, clear communication, and strong emergency plans help support safe sedation.
Comprehensive Medical History Review

You should expect a detailed review of your medical history before any form of dental sedation. This step is not optional. It helps your dentist decide if in-office sedation is appropriate for you.
Your provider will review:
- Heart conditions, including high blood pressure or arrhythmias
- Lung disease, such as asthma or COPD
- Diabetes and blood sugar control
- Sleep apnea
- Kidney or liver disease
- Past reactions to anesthesia
You should also share past hospitalizations, surgeries, and any problems with prior dental anesthesia. Even small details matter. Clear and honest answers help your dental team lower risk and plan for safe sedation.
Medical and Medication Consultations
If you have a complex medical condition, your dentist may contact your physician before scheduling sedation. This step is common for patients with heart disease, bleeding disorders, or uncontrolled diabetes.
Some patients with higher medical risk need medical clearance. The American Society of Anesthesiologists notes that patients with major medical problems may need evaluation before a procedure in office-based settings.
You must also provide a full list of medications, including:
- Blood thinners
- Insulin or oral diabetes drugs
- Blood pressure medication
- Anti-anxiety drugs
- Herbal supplements
Certain drugs can increase bleeding, affect blood pressure, or interact with sedatives. Your dentist may adjust the sedation plan or timing of your dose. These steps protect you during dental sedation services.
Monitoring and Emergency Preparedness
Safe sedation depends on close monitoring during the procedure. A trained team member must watch your vital signs the entire time.
Your team will track:
- Heart rate
- Blood pressure
- Oxygen levels
- Breathing pattern
For deeper levels of dental anesthesia, monitoring becomes even more strict. Equipment must match current safety standards, and emergency drugs and airway tools must stay ready for immediate use.
Your dental office should maintain resuscitation training such as Basic Life Support (BLS), and in some settings Advanced Cardiac Life Support (ACLS) or Pediatric Advanced Life Support (PALS). Staff should check emergency equipment on a regular schedule.
When you choose a provider who follows structured safety protocols, you lower the chance of preventable complications during dental sedation services.
Looking for safe sedation dentistry? Fill out our new patient form and book your visit today.
Sedation Dentistry for Special Needs and Accessibility
You may face extra barriers when you or your loved one has physical, cognitive, or sensory challenges. Sedation dentistry for special needs patients can reduce stress, improve safety, and make dental care more consistent and predictable.
Sedation for Patients With Sensory or Behavioral Challenges
If you live with autism, ADHD, intellectual disabilities, or severe dental anxiety, routine dental visits can feel overwhelming. Bright lights, loud sounds, and strong smells may trigger distress or behavioral reactions.
Conscious sedation helps you stay relaxed while still breathing on your own and responding to simple instructions. Dentists often use oral medication or nitrous oxide for mild to moderate anxiety. These methods lower movement and improve cooperation without full general anesthesia.
Many practices now focus on sedation dentistry for patients with special needs to make care more manageable. This approach supports patients with intellectual or developmental disabilities who struggle with traditional visits.
Sedation also allows your dentist to complete more treatment in fewer appointments. That means fewer stressful trips and better long-term oral health.
Improving Dental Access and Comfort for All
Access to dental care remains a major issue for people with disabilities. Some clinics lack trained staff or proper equipment, which limits safe treatment options.
The field of Special Care Dentistry focuses on patients with medical, physical, or cognitive conditions. It promotes coordinated care and proper training so providers can adjust treatment plans to your specific needs.
Sedation dentistry for special needs patients improves access by:
- Reducing fear and dental anxiety
- Allowing longer or more complex procedures
- Lowering the need for hospital-based general anesthesia
- Supporting safer in-office treatment
Clinics may adjust lighting, scheduling, and communication methods. When combined with conscious sedation, these changes make visits calmer and more predictable.
You deserve care that respects your health status, comfort level, and communication style.
Role of Caregivers in Coordination
Caregivers play a key role in safe and effective sedation. You help the dental team understand medical history, medications, allergies, and behavior patterns.
Before the appointment, you should review:
| Topic | Why It Matters |
| Current medications | Some drugs interact with sedatives |
| Medical diagnoses | Conditions may change sedation choice |
| Past sedation history | Prior reactions guide safer planning |
| Communication needs | Helps the team prepare supports |
You also help monitor recovery after the visit. Clear written and verbal instructions reduce confusion and improve safety.
When caregivers, dentists, and medical providers communicate well, sedation dentistry for special needs patients becomes more predictable and less stressful for everyone involved.
Benefits and Considerations for Long-Term Dental Health
Sedation dentistry can help you stay consistent with care, even if you have complex health needs. It supports regular visits, lowers stress, and allows your dentist to treat problems before they grow worse.
Reducing Dental Anxiety for Medically Complex Patients

If you live with heart disease, diabetes, or a neurologic condition, dental visits may feel stressful. Dental anxiety can raise your heart rate and blood pressure, which may affect your overall health.
Sedation helps you stay calm and still during treatment. This is especially helpful if you have limited mobility, tremors, or difficulty sitting for long periods. Dentists adjust medications based on your age, weight, and medical history.
With safe sedation, you reduce fear-based delays. That means fewer canceled visits and fewer untreated infections that could affect your heart or blood sugar levels.
Enabling Preventive and Restorative Care
When anxiety keeps you from the dentist, small problems can turn into larger ones. Sedation makes it easier for you to complete cleanings, colored-fillings, and even longer procedures in one visit.
You may also benefit if you have cognitive decline or limited cooperation. A review of sedative agents for patients with special needs explains how dentists match the drug and level of sedation to your medical status.
This careful approach allows your dentist to:
- Remove decay before it spreads
- Treat gum disease early
- Repair broken teeth before infection develops
By staying on schedule with preventive care, you lower your risk of tooth loss and avoid emergency visits. That protects both your oral health and your overall medical stability.
Long-Term Safety and Outcomes
Your safety depends on detailed planning. Before sedation, your dentist reviews your medical history, current medications, and recent lab results if needed. They may consult your physician, especially if you have heart, lung, or kidney disease.
During treatment, the team tracks your oxygen level, pulse, and blood pressure. These steps support safe sedation and reduce the risk of breathing or heart problems.
When your dental care stays consistent, you face fewer infections and less chronic inflammation. Over time, that steady care supports better long-term dental health and helps you manage your medical conditions with fewer complications.
Frequently Asked Questions
Medical conditions like heart disease, asthma, diabetes, and sleep apnea can change how your body responds to sedation. Your dentist will review your health history, current symptoms, and medications to choose the safest option for you.
What medical conditions could impact the suitability of sedation dentistry?
Heart disease, high blood pressure, and irregular heart rhythms can affect how your body handles sedative drugs. Sedation can change your heart rate and blood pressure, so your dentist must plan with care.
Respiratory conditions like asthma or chronic obstructive pulmonary disease (COPD) also matter. Sedation can slow breathing, which may increase risk if you already have lung problems.
Obstructive sleep apnea raises concern because sedation relaxes airway muscles.
Liver or kidney disease can affect how your body breaks down and clears medications. Diabetes may also require careful timing of meals and insulin before your visit.
How does a dentist assess if a patient with a medical condition is fit for sedation?
Your dentist will review your full medical history. You should list all diagnoses, past surgeries, and hospital stays.
They will also review your current medications and any allergies. Some offices may request medical clearance from your physician before treatment.
During the visit, the team checks your blood pressure, heart rate, and oxygen levels.
Are there alternative calming methods for patients with medical conditions who can’t have sedation?
Yes, you still have options if sedation is not advised.
Your dentist may use local anesthesia alone to numb the treatment area. This controls pain without affecting your whole body.
You can also try behavioral techniques such as guided breathing, music, or shorter appointments. Some offices offer comfort items like blankets or allow a support person in the room to help you feel at ease.
What are the potential risks of sedation dentistry for patients with specific medical conditions?
Sedation can lower blood pressure or slow breathing. For patients with heart or lung disease, these effects may pose higher risk.
People with sleep apnea may have airway blockage during deeper sedation. Patients with liver or kidney disease may process drugs more slowly, which can extend recovery time.
Reviews of common concerns and risks of dental sedation explain that careful screening helps reduce these problems. Your dentist lowers risk by adjusting the drug type and dose to fit your condition.
How should patients with medical conditions prepare for a sedation dentistry appointment?
Follow all pre-visit instructions closely. You may need to avoid food and drinks for several hours before your appointment.
Take only the medications your dentist approves on the day of treatment. Bring a full list of your prescriptions and dosages.
Arrange for a responsible adult to drive you home if you receive oral or IV sedation. Plan to rest for the remainder of the day.
Can ongoing medications affect the type of sedation used in dentistry for a patient with medical conditions?
Yes, many medications can interact with sedatives.
Blood thinners may affect bleeding during certain procedures. Drugs for anxiety, depression, or seizures can change how sedatives work in your body.
Insulin and other diabetes medications require careful timing if you must fast before treatment. Always tell your dentist about every prescription, over-the-counter drug, and supplement you take so they can select the safest sedation method for you.